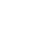Anticipate, Assist, Resolve: Agentic AI and Proactive Member Engagement in Healthcare
Healthcare is undergoing a pivotal transformation—driven by the urgent need to elevate member engagement as a cornerstone of financial resilience, regulatory alignment, and brand credibility. Contact centers, once viewed as operational backstops, are now emerging as strategic assets that shape the member experience.
With Medicare Star Ratings placing significant weight on experience metrics, organizations must reimagine how they connect with members. Fragmented workflows and impersonal automation are no longer viable. What’s needed is not just better technology—but a bold shift in architecture that prioritizes empathy, agility, and integration.
This is a moment to lead with vision: to design systems that not only meet expectations but redefine them.
As contact centers evolve from operational support to experience orchestrators, the need for intelligent, adaptive systems becomes urgent.
Agentic AI represents a new class of autonomous technology—capable of reasoning, adapting, and acting independently across complex, regulated environments. Unlike rule-based bots or scripted IVRs, Agentic AI brings contextual intelligence, emotional acuity, and decision logic to the deeply human domain of healthcare.
The strategic case is compelling. With a projected market growth from $538.51 million in 2024 to $4.96 billion by 2030—a CAGR of 45.56%—Agentic AI is not just innovation; it’s a competitive differentiator. For payers managing Medicaid, Medicare, and ACA populations, it offers a pathway to scalable empathy, operational resilience, and experience-led compliance.
The Engagement Crisis: An Economic and Structural Fault Line
When Experience Becomes a Revenue Driver
Member satisfaction is no longer a soft metric. With Medicare Star Ratings assigning 57% of their scoring to experience and complaints, poor engagement translates directly into lost Quality Bonus Payments and market erosion. Net Promoter Scores (NPS) in healthcare average around 38—far below industries like tech, where 70+ is standard. This is not just a service gap. It’s a systemic vulnerability with clear revenue implications.